THE AGING OF WYOMING: State’s ‘Aging Society’ Expected to Cause Medicaid Costs to Soar
Lawmakers consider lifting restrictions on new nursing homes
- Published In: Other News & Features
- Last Updated: Jun 30, 2023

Community members and dignitaries celebrated the grand opening of the state of Wyoming’s new skilled nursing facility for veterans in Buffalo last fall. The state expects to see rising demand for nursing home beds in the coming years, as the population ages. (Courtesy photo from Sgt. Kristina Kranz of the U.S. Army National Guard)

By CJ Baker
Special to the Wyoming Truth
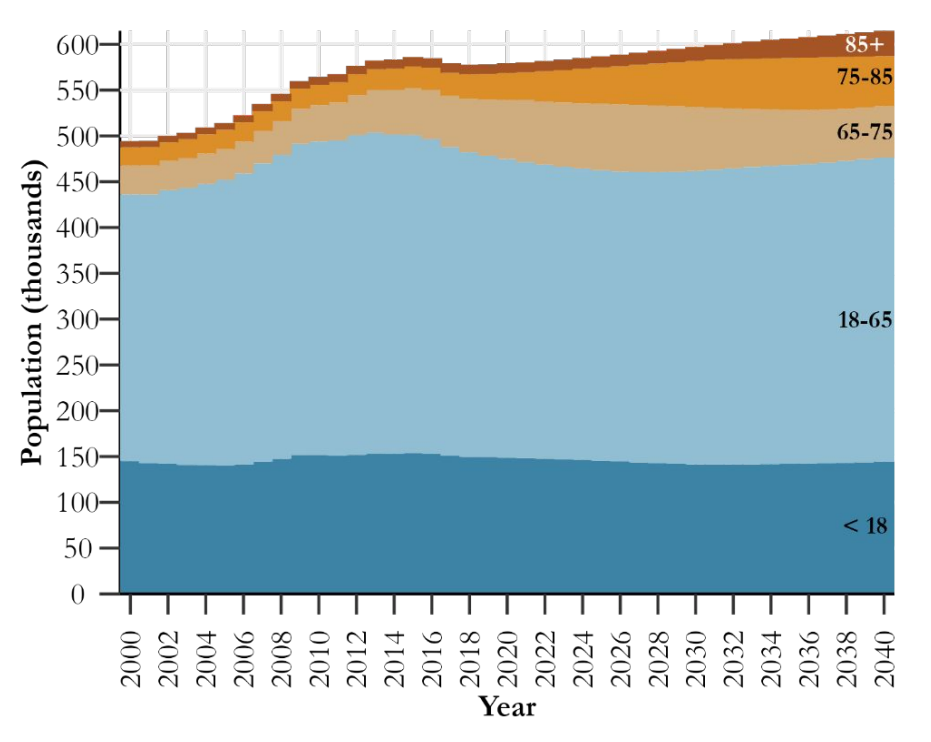
Wyoming’s population is getting older and sicker — and state officials say the shift is poised to stretch both the state’s budget and its long-term care providers.
“… We are sort of an aging society,” Wyoming Department of Health data analyst Franz Fuchs reported to the Legislature’s Joint Labor, Health & Social Services Committee this month.
About half of the state’s growing population of seniors will wind up needing professional long-term care, and much of that care winds up being paid for by Wyoming Medicaid. As a result, the program’s annual costs for long-term care are projected to roughly double by 2040 — from about $136 million today to as much as $275 million.
Additional investment may be needed in the state’s nursing homes, too, as the department expects the demand for beds to exceed the existing capacity in the coming years.
“Scary,” Committee Co-Chair Rep. Dan Zwonitzer (R-Cheyenne) remarked when Fuchs wrapped up his June 22 presentation.
The panel won’t dig into the long-term care issue until a meeting this fall, but some lawmakers already know they want to repeal a state law that requires nursing home to obtain a “certificate of need” from the state before starting up or expanding.
“I think this is a no-brainer,” Rep. Jeanette Ward (R-Casper) said in moving to end the requirement.
“It artificially controls the market,” she said, “and I think we would benefit from a free market.”
At its meeting in Evanston, the committee agreed to consider a repeal, but some lawmakers and officials said the state would be better off making more modest tweaks.
Question of need
The rationale behind the decades-old statute was to avoid an oversupply of nursing homes and to encourage the development of home-based care, which is significantly cheaper and preferred by residents, said Wyoming Department of Health Director Stefan Johansson. Wyoming Medicaid pays an average of $59,172 a year for members living in a nursing home, versus $22,452 for those in assisted living facilities or receiving home-based care; the state splits those rising costs with the federal government.
Under Wyoming’s certificate of need statute, a new nursing home can only be constructed if the other facilities in the area are above 85% occupancy. Similarly, unless that 85% threshold is exceeded, existing nursing homes can add no more than 10 beds within a two-year period.

Since 2009, the Department of Health has received 18 requests to build new nursing homes and denied seven because they didn’t meet the occupancy criteria. Two facilities were cleared to expand beyond the 10-bed/10% cap, though only one did so.
Wyoming Hospital Association President Eric Boley said the limits don’t always make sense. For instance, some designs call for expansions to be done 12 beds at a time rather than 10.
Still, Boley expressed unease about a full repeal; removing that requirement for hospitals proved unwise, he argued, leading the construction of some new facilities that “cherry picked” which services they would offer.
“We have some really, really good nursing homes in our state and I worry about repealing certificate of need completely at this point, because those nursing homes need protection,” Boley said. “And in all honesty, most of them are struggling mightily right now.”
In Buffalo, the state recently built a skilled nursing facility for veterans that wasn’t subject to the requirements, and Boley said both it and the existing nursing home operated by Johnson County Healthcare Center are now struggling to find enough staff.
“I do think there needs to be some measures in place to make sure that existing facilities can take care of the patients in their facilities,” he said.
For her part, Ward argued that a repeal “increases competition, which generally is a good thing for the consumer.”
“If it’s good for kids in education, it’s good for old people in nursing homes,” Zwonitzer wryly offered, referencing the ongoing debates over alternatives to the traditional K-12 education system.
Temporary drop in demand
If the state scraps its certificate of need requirement, Johansson and Boley said it’s unclear whether the change would actually lead to the construction of new nursing homes.

Demand for beds dipped with the COVID-19 pandemic, partly because of the deaths that occurred in nursing homes and among the elderly, but also because of an apparent “reluctance to enter long-term care to begin with,” Fuchs said.
Since 2015, more Wyoming Medicaid members have opted for home-based care or assisted living facilities over nursing homes. The preference has become especially pronounced in recent years. There’s currently an average of 2,425 members on the community choices waiver each month, as compared to 1,385 monthly members in nursing homes (who represent roughly 65% of all bed-days in the state).
However, Fuchs said the demand for nursing home beds is expected to rebound and exceed the current capacity in the coming years, as the number of senior citizens in the state continues to grow.
“We are getting older faster than any state,” Tom Lacock, the associate state director of AARP Wyoming, told the committee. “But we’re also really struggling to keep our younger generation in the state.”
While that “brain drain” poses problems for Wyoming’s workforce, it’s also an issue when it comes to long-term care, as children often become unpaid caregivers for their aging parents.
“So … when we lose that younger generation, that burden really tends to fall onto the state,” Lacock said.
The committee will revisit the topic of long-term care at its Sept. 21-22 meeting in Saratoga.













